Can Exoskeletons Reduce Musculoskeletal Disorders in Healthcare Workers?
Posted on by
Musculoskeletal Disorders (MSDs) remain a major concern for workers in the healthcare industry. Healthcare workers are at high risk of work-related MSDs mainly caused by overexertion from lifting and moving patients (i.e., patient handling). Wearable robots—exoskeletons or exosuits—may be a useful tool to help reduce risk of MSDs during patient handling.
Background
Based on the Bureau of Labor Statistics (BLS) data, hospital workers have nearly twice the rate of overexertion injuries when compared to the average rate of overexertion injuries for all industries [1]. In 2017, there were about 3 million registered nurses, 0.8 million home health aides and 1.5 million nursing assistants [2-4]. Nursing assistants alone reported 18,090 MSD cases in 2017 (over 5% of the total MSD cases) [5]. More than half of these MSD cases involved back injuries [6]. In addition, the vast majority of these healthcare workers are women (only about 10% of registered nurses and 11% of nursing and home health aides are men) [7], who generally have less physical strength than male workers.
The safety of workers and patients are both at stake whenever a patient is lifted or moved. Manual handling without assistance imposes unacceptable risk of injury not only to the worker but also the patient if they are dropped while being moved. The Food and Drug Administration’s (FDA) Manufacturer and User Facility Device Experience Database (MAUDE) has documented adverse events including serious injuries and deaths, particularly to patients, during the use of standard patient handling equipment [8]. The consequences of such incidents are exceptionally costly and sometimes irreversibly tragic. Furthermore, the occurrence of adverse events might increase due to the rapidly aging population, the higher prevalence of obesity, and the shortage and aging of the healthcare workforce in the future [9-10].
As current recommendations, Safe Patient Handling and Mobility (SPHM) programs involving the use of mechanical equipment and safety procedures have demonstrated significant reductions in the injury rate of patient care workers (see NIOSH website on this topic). Despite successes with these programs, laws requiring SPHM programs in healthcare exist in only 11 of 50 states and no federal legislation has been passed to mandate safe patient handling programs [11]. Additionally, certain specialized healthcare settings—such as home healthcare (see related NIOSH blog), long term care facilities, operating rooms, and imaging/radiology facilities—present unique challenges to adopting the SPHM programs [12]. When working in such “uncontrolled” environments and tight spaces, it is often not possible to avoid manual patient handling with limited or no ergonomic assist equipment. While we expect continuous progress with SPHM programs, the high incidence rates of MSDs among patient care workers show that we still face severe challenges. Thus, we need to improve the existing intervention methods and explore non-traditional assistive technologies.
Are Exoskeletons the Answer?
There is an ongoing movement towards human-robot collaboration in modern industry. Using wearable robots (exoskeletons or exosuits) can provide the benefits of robots while retaining the flexibility of humans. Various wearable robots enhance workers’ strength, endurance and performance (see potential benefits and risks discussed in a NIOSH blog on Industrial Exoskeletons). Particularly, promising results were shown in the material handling industry [13].
The development of exoskeletons for safe patient handling is in its infancy. There are several challenges anticipated for exoskeleton applications in a healthcare setting, including but not limited to:
- unique “object-handling” tasks: such as irregular and complex geometry of the lift and versatile task demands including the ability to react quickly to sudden situations
- patient comfort and safety: exoskeletons should not affect speed and smoothness of handling motions
- designs for women: exoskeleton users are mostly women, but the majority of existing exoskeletons were designed for men in other male-dominant industries. Women may have different requirements for exoskeleton’s static and dynamic fit.
- limited workspaces with various medical equipment: exoskeletons cannot interfere with other medical devices
- disinfection: exoskeletons require easy disinfection for safety of both workers and patients
- other social and culture considerations: such as whether exoskeletons influence interaction and trust between the worker and the patient
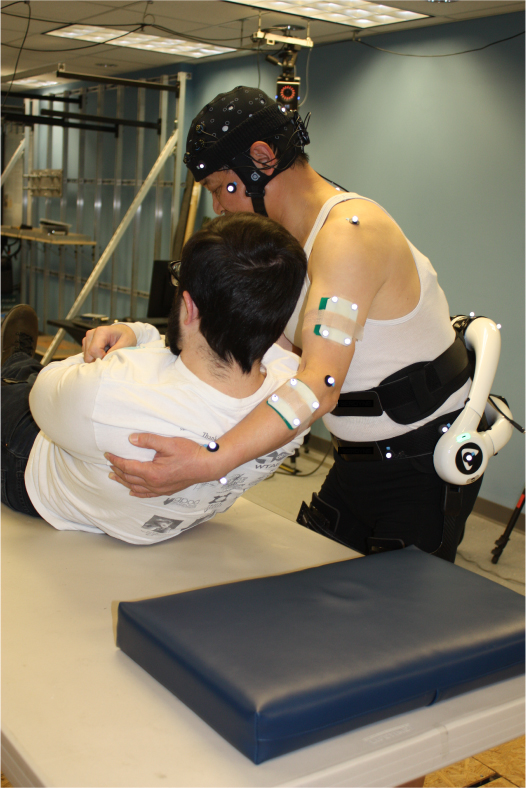
NIOSH scientists are actively searching for exoskeletons that are specifically designed for healthcare workers, while simultaneously developing evaluation methods to assess the feasibility of introducing this emerging technology into patient handling. NIOSH researchers conducted pilot testing to evaluate potential exoskeletons by assessing the physiological and psychophysical responses of the users while performing simulated patient handling tasks (shown in pictures). The effects of exoskeletons on the pressure or “load” at users’ joints—which cannot be measured directly—are examined using biomechanical models. Advanced Artificial Intelligence (AI) approaches will be incorporated to develop comprehensive evaluation methods for assessing merits and residual risks of various styles of exoskeletons. The program strives to propose the basic criteria and method for evaluating exoskeleton systems in patient handling and provide a foundation for future large-scale laboratory and onsite studies.
Although the current wearable-robot technology is not expected to be used in all patient handling tasks, we need to evaluate if this technology could be introduced to uncontrolled or specialized healthcare environments, or if it could complement the existing SPHM programs. Nevertheless, innovative and “smart” exoskeleton products are in great demand to help reduce work-related MSDs for healthcare workers and enhance safety and quality of care for patients.
If you have experience with viable wearable robots for patient handling, please comment below or contact Dr. Liying Zheng (lzheng2@cdc.gov).
Liying Zheng, PhD, is a Research Biomechanical Engineer in the Physical Effects Research Branch in the NIOSH Health Effects Laboratory Division.
 This blog is part of a series hosted by NIOSH to commemorate nurses during the Year of the Nurse.
This blog is part of a series hosted by NIOSH to commemorate nurses during the Year of the Nurse.
Other blogs in the series include:
- Year of the Nurse
- Managing Fatigue During Times of Crisis: Guidance for Nurses, Managers, and Other Healthcare Workers
- Nurses’ and Other Health Professionals’ Wellness and Safety Resource Update
- Surgical Smoke Inhalation: Dangerous Consequences for the Surgical Team
- Safety Culture and Health Care
- Work Ability among Older Nurses
- The Unique Occupational Environment of the Home Healthcare Worker
- Preventing Needlesticks and Sharps Injuries: Reflecting on the 20th Anniversary of the Needlestick Safety and Prevention Act
- Celebrating Nurses
References
[1] BLS. Injuries, Illnesses, and Fatalities; TABLE R8. Incidence rates for nonfatal occupational injuries and illnesses involving days away from work per 10,000 full-time workers by industry and selected events or exposures leading to injury or illness, private industry. 2017; Available from: https://www.bls.gov/iif/oshwc/osh/case/cd_r8_2017.htm.
[2] BLS. Occupational Employment and Wages, 29-1141 Registered Nurses. 2017; Available from:
https://www.bls.gov/oes/2017/may/oes291141.htm
[3] BLS. Occupational Employment and Wages, 31-1011 Home Health Aides. 2017; Available from:
https://www.bls.gov/oes/2017/may/oes311011.htm
[4] BLS. Occupational Employment and Wages, 31-1014 Nursing Assistants. 2017; Available from:
https://www.bls.gov/oes/2017/may/oes311014.htm
[5] BLS. 2017 Survey of Occupational Injuries & Illnesss Charts Package. 2018; Available from: https://www.bls.gov/iif/osch0062.pdf.
[6] BLS. Back injuries prominent in work-related musculoskeletal disorder cases in 2016. The Economics Daily 2018; Available from: https://www.bls.gov/opub/ted/2018/back-injuries-prominent-in-work-related-musculoskeletal-disorder-cases-in-2016.htm.
[7] BLS. Labor Force Statistics from the Current Population Survey; Table 11. Employed persons by detailed occupation, sex, race, and Hispanic or Latino ethnicity. 2017; Available from: https://www.bls.gov/cps/cpsaat11.htm.
[8] Elnitsky, C.A., J.D. Lind, D. Rugs and G. Powell-Cope, Implications for patient safety in the use of safe patient handling equipment: a national survey. Int J Nurs Stud, 2014. 51(12): p. 1624-33.
[9] US Census Bureau. U.S. Census Bureau Projections Show a Slower Growing, Older, More Diverse Nation a Half Century from Now. 2012; Available from: https://www.census.gov/newsroom/releases/archives/population/cb12-243.html.
[10] Buerhaus, P.I., Current and future state of the US nursing workforce. JAMA, 2008. 300(20): p. 2422-4.
[11] Weinmeyer, R., Safe Patient Handling Laws and Programs for Health Care Workers. AMA J Ethics, 2016. 18(4): p. 416-21.
[12] National Occupational Research Agenda (NORA). The lastest agenda for Healthcare and Social Assistance. 2019; Available from: https://www.cdc.gov/nora/councils/hcsa/pdfs/National_Occpational_Agenda_for_HCSA_February_2019-508.pdf
[13] de Looze, M.P., T. Bosch, F. Krause, K.S. Stadler and L.W. O’Sullivan, Exoskeletons for industrial application and their potential effects on physical work load. Ergonomics, 2016. 59(5): p. 671-81.
Posted on by

