Advanced Sensor Technologies and the Future of Work
Posted on by
Measuring worker exposure to hazardous substances is a key step to reducing risk and protecting workers. Sensors used in the workplace provide exposure data to inform prevention measures. Newer sensor technologies have the potential to greatly accelerate advances in occupational exposure science. A new commentary, Advanced Sensor Technologies and the Future of Work, in the American Journal of Industrial Medicine discusses some of the benefits and challenges of advanced sensor technologies. Key points from the commentary are summarized below.
Background
Exposure measurement has come a long way. Beginning in the mid-1930s, occupational exposure science was based on a two-step strategy—collecting air samples from the work environment followed by laboratory analysis using standardized methods.[1] The advent of the personal sampler in 1960 demonstrated that area sampling can underestimate worker exposures.[2] Since then, personal sampling has become accepted practice in occupational hygiene.[1] Today, personal sampling is still dependent on subsequent laboratory analysis for actionable results resulting in a delay in implementing mitigation strategies.[3]
The need to detect hazardous exposures in time to rapidly mitigate harmful effects led to the development of “direct reading” devices that can detect the presence of a chemical or physical hazard. The hazard interacts with the sensor either by a periodic or continuous process, and the analytical results are delivered in “real time,” or at the end of a shift, or can alarm at preset hazard levels so that the individual can then mitigate the exposure. [3,4] Examples of direct reading devices include the pocket radiation dosimeter patented in 1935 and the noise dosimeter first patented in the 1950s as well as modern devices such as field-portable, real-time sensor devices like gas and vapor monitors; real-time aerosol monitors; X-ray fluorescence detectors for metals; and immunochemical assay kits for methamphetamines, microorganisms, and other kinds of immunologically active contaminants. [3, 5-7] Newer direct-reading sensor devices are incorporating recent advances in electrochemical, optical or mechanical transducers, nanomaterials, electronics miniaturization, portability, batteries with high-power density, wireless communication, energy-efficient microprocessing, and display technology. [8-9]
Advanced Sensor Technologies
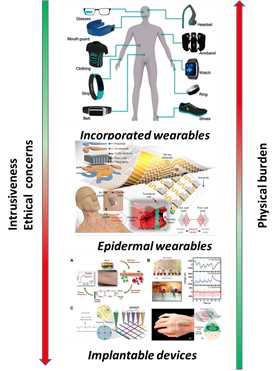
There are three broad categories of advanced sensor technologies—placeable, wearable, and implantable devices.
Placeable sensors can be placed in and around the workplace to collect information from the ambient work environment. These sensors have a long history in the workplace and have been used to detect worker occupancy, movement within the workplace, and a variety of atmospheric factors. New opportunities and applications for placeable sensors involve networks of multiple sensor nodes distributed around a workplace that can measure the same or several different hazards. As a new occupational exposure assessment strategy, wireless area sensor networks can overcome the low sample size limitations of personal sampling by monitoring multiple analytes in real time, be more cost-effective than personal sampling methods, and can characterize the distribution of hazards with a high degree of spatiotemporal resolution. [13] The challenge facing wireless placeable sensor networks continuously collecting information from many micro-sensor nodes is how to efficiently process the data coming from each node into timely, actionable information. The newest application of wireless area sensor networks is the wireless body sensor network using wearable instead of placeable sensors.[14]
Wearable sensors can be worn on or over clothing such as vests; attached to safety helmets; incorporated into footwear; worn as smart eyeglasses or contact lenses; or placed in the external auditory canal. [15-16] Optimizing the location of attached wearables depends on the sensor’s monitoring purpose, need for interaction between the sensor controls and the worker, display reachability, weight, and worker acceptance. [17] Wearable sensor technologies are not without risk. Physical hazards presented by wearable technologies can include:
(1) dermal irritation if exposure to the chemicals contained in device occurs,
(2) chemical burns if a battery leaks a reactive material,
(3) thermal burns if a wearable battery suddenly discharges its stored energy, or
(4) auditory damage if an implanted audio device malfunctions or “plays” a signal from another source.
In addition to risks inherent to sensors, several barriers to adoption of sensor technologies have been identified among safety professionals—sensor durability, good manufacturing practices, the cost-benefit ratio for implementation, concerns about worker acceptance, and employer and worker conformance with a sensor’s intended use.
Future applications of wearable sensors include sensors that are woven into textiles that can be worn by a worker as clothing (electronic textile wearables) and sensors incorporated in thin “skin-like” films or tattoos that can be applied directly to the epidermis (electronic epidermal wearables). [18]
Wearable textile sensors represent a merging of material science and electronics to embed electronic circuitry within textiles to create a new class of textiles called smart textiles, intelligent textiles, or electronic or e-textiles. These sensors can sense changes in the ambient environment, like clothing integrated with gas sensors or those measuring human internal chemical parameters or sample human perspiration non-invasively and on a continuous basis.[18-19] While e-textiles are a promising type of wearable sensor technology, there are many technical challenges to their commercial or workplace application. These challenges include analytical requirements, power supply, data acquisition and processing, communication, and maintaining the functionality of epidermal materials during use in relevant environments. Despite these challenges, e-textiles may soon play a role in the future of work.
Electronic epidermal wearables are ultra‐thin, “skin‐like” membranes, with tattoo‐like conformability and stretchability that can non‐invasively collect physiological information from within the body through the epidermis.[20] Epidermal wearable sensors are now being investigated to measure pH, various electrolytes, and other metabolites on or under the skin physically, chemically, or electrochemically as point‐of‐care applications. Electronic epidermal and transdermal wearables may have a role in detecting biomarkers of occupational exposure and disease in the future of work. Electronic epidermal wearables are advanced enough to facilitate physiologic monitoring of heart rate, respiration, core body temperature, body water loss, and estimation of thermal load to identify developing heat stress.
Implantable sensors (i.e., a cardiac pacemaker) can be inserted into the skin via microneedles, microchips, or can be ingested. [9,21-22] These sensors can provide more accurate measurements. The ingestible sensor has the greatest likelihood of moving from research into clinical and workplace applications. For example, as a clinical tool, an ingestible sensor can gather images of the intestines and sample enzymes, metabolites, hormones, and the microbiome. There are limitations including the perception from workers that this is an invasive medical procedure, raising ethical and legal issues.
Moving Forward
Acceptance of environmental and physiological sensors by workers depends on how well employers and occupational safety and health professionals partner with workers to introduce fully transparent sensor-technology-based programs.[23] To ensure successful adoption of sensor technologies in the workplace of the future, best practice recommendations include:
(1) making participation in sensor monitoring voluntary and not coercive,
(2) ensuring all sensor data that are used is transparent to the worker,
(3) utilizing only sensors that have been validated by interventional effectiveness studies before being applied in the workplace, and
(4) ensuring that data collection is limited to working hours.
Importantly, all data outputs should conform to the latest secured data transmission governance and stored under robust cybersecurity protections. [24]
As new sensor technologies advance occupational exposure science there is the potential for improved worker safety and health. As these technologies move from the research laboratory into the workplace, we need to be aware of both the benefits and challenges they present for workers, employers and safety and health practitioners. While sensors may make exposure assessment more convenient and comprehensive, the intrusiveness that accompanies extensive worker monitoring needs to be balanced by a respect for privacy and trust that personal health data remains secure. Additionally, there needs to be a collaborative agreement between sensored workers and their employers that any advanced sensor technology introduced into the workplace directly benefits worker safety and health.
Please share with us your experiences with workplace sensors and your thoughts for their application in the future of work.
John Howard, MD, is the Director of the National Institute for Occupational Safety and Health.
Vladimir Murashov, PhD, is a Senior Scientist in the NIOSH Office of the Director.
Emanuele Cauda, PhD, is a Research Engineer in the NIOSH Pittsburgh Mining Research Division and co-Director for the NIOSH Center for Direct Reading and Sensor Technologies.
John Snawder, PhD, DABT, is a Research Toxicologist in the NIOSH Health Effects Laboratory Division and Co-Director of the NIOSH Center for Direct Reading and Sensor Technologies.
For more information see the Center for Direct Reading and Sensor Technologies website.
References
- Fenske RA. For good measure: origins and prospects of exposure science (2007 Wesolowksi Award Lecture). J Expo Sci Env Epid. 2010;20:493‐502. doi:10.1038/jes.2010.26.
- Sherwood RJ, Greenhalgh DMS. A personal air sampler. Ann Occup Hyg. 1960;2:127‐132.
- Pearce T, Coffey C. Analytical performance issues: integrating direct‐reading exposure assessment methods into industrial hygiene practice. J Occup Environ Hyg. 2011;8(5):D31‐D36. doi:10.1080/15459624.2011.569314.
- Cauda E & Hoover M Right Sensors Used Right: A Life‐Cycle Approach for Real‐Time Monitors and Direct Reading Methodologies and Data. Washington, DC: National Institute for Occupational Safety and Health, Centers for Disease Control and Prevention, US Dept of Health and Human Services; 2019. Accessed September 27, 2021. https://blogs.cdc.gov/niosh-science-blog/2019/05/16/right-sensors-used-right/. Accessed October 11, 2021.
- National Institute for Occupational Safety and Health. Components for evaluation of direct‐reading monitors for gases and vapors. A NIOSH Technical Report, Publication No. 2012–162. Washington, DC: National Institute for Occupational Safety and Health, Centers for Disease Control and Prevention, US Dept of Health and Human Services; 2012. Accessed September 27, 2021. https://www.cdc.gov/niosh/docs/2012-162/pdfs/2012-162.pdf
- Baron PA. Direct‐reading instruments for aerosols. A review. Analyst. 1994;119(1):35‐40. doi:10.1039/an9941900035
- Laohaudomchok W, Cavallari JM, Fang SC, et al. Assessment of occupational exposure to manganese and other metals in welding fumes by portable X‐ray fluorescence spectrometer. J Occup Env Hyg. 2010;7(8):456‐465. doi:10.1080/15459624.2010.485262
- Seshadri DR, Li RT, Voos JE, et al. Wearable sensors for monitoring the physiological and biochemical profile of the athlete. NPJ Digit Med. 2019;2:72‐88. doi:10.1038/s41746-019-0150-9
- Tarar AA, Mohammad U, Srivastava SK. Wearable skins sensors and their challenges: a review of transdermal, optical, and mechanical sensors. Biosensors. 2020;10(6):56‐78. doi:10.3390/bios10060056
- National Academies of Sciences, Engineering and Medicine. Exposure science in the 21st century: a vision and a strategy. National Academies Press; 2012. doi:10.17226/13507
- Goede H, Kuijpers E, Krone T, et al. Future prospects of occupational exposure modelling of substances in the context of timeresolved sensor data. Ann Work Expos Health. 2021;65(3):246‐254.doi:10.1093/annweh/wxaa102
- Ozanich R. Chem/bio wearable sensors: current and future direction. Pure Appl Chem. 2018;90(10):1605‐1613. doi:10.1515/pac-2018-0105
- Zuidema C, Stebounova LV, Sousan S, et al. Estimating personal exposures from a multi‐hazard sensor network. J Expos Sci Environ Epidemiol. 2020;30(6):1013‐1022. doi:10.1038/s41370-019-0146-1
- Khan RA, Parthan AK. The state‐of‐the‐art wireless body area sensor networks: a survey. Int J Distrib Sens Netw. 2018;14(4):2‐23. doi:10.1177/15501477187689994
- Lee JH, Kim H, Hwang J‐Y, et al. 3D printed, customizable, and multifunctional smart electronic eyeglasses for wearable healthcare systems and human–machine interfaces. ACS Appl Mater Interfaces. 2020;12(19):21424‐21432. doi:10.1021/acsami.0c03110
- Park J‐H, Jang D‐G, Park JW, Youm S‐K. Wearable sensing of inear pressure for heart‐rate monitoring with a piezo‐electronic sensor. Sensors. 2015;15(9):23401‐23417. doi:10.3390/s150923402
- Zeagler C. Where to wear it: functional, technical, and social considerations in on‐body location for wearable technology 20 years of designing for wearability. In: Proceedings of the 2017 ACM International Symposium on Wearable Computers; 2017:150‐157. doi:10.1145/3123021.3123042
- Gualandi I, Tessarolo M, Mariani F, Possanzini L, Scavetta E, Fraboni B. Textile chemical sensors based on conductive polymers for the analysis of sweat. Polymers. 2021;13(6):894‐917. doi:10.3390/polym13060894
- Cherenack K, von Pieterson L. Smart textiles: challenges and opportunities. J Appl Physics. 2012;112(9):091301. doi:10.1063/1.4742728
- Amendola S, Occhiuzzi C, Miozzi C, et al. UHF epidermal sensors: technology and applications. In: Sazonov E, ed. Wearable Sensors: Fundamentals, Implementation and Applications. 2nd ed. Elsevier; 2021:133‐161. doi:10.1016/B978-0-12-819246-7.00005-X
- Zhang JXS, Hoshino K. Molecular Sensors and Nanodevices: Principles,Designs and Applications in Biomedical Engineering. William Andrew; 2014:415‐465. https://www.elsevier.com/books/molecular-sensors-and-nanodevices/zhang/978-0-12-814862-4
- Guk K, Han G, Lim J, et al. Evolution of wearable devices with real‐time disease monitoring for personalized healthcare. Nanomaterials‐Basel. 2019;9:813‐837. doi:10.3390/nano9060813
- Yaseen M, Saleem K, Orgun MA, et al. Secure sensors data acquisition and communication in eHealthcare: review on the state of the art. Telemat Inform. 2018;35(4):702‐726. doi:10.1016/j.tele.2017.08.005
- le Feber M, Jadoenathmisier T, Goede H, Kuijers E, Pronk A. Ethics and privacy considerations before deploying sensor technologies for exposure assessment in the workplace: results of a structured discussion amongst Dutch stakeholders. Ann Work Expo Health. 2021;65(1):3‐10. doi:10.1093/annweh/wxaa093
Posted on by

