AFM is Serious: Know the Symptoms. Act Fast.
Posted on by
Acute flaccid myelitis (AFM) is a serious neurologic condition that causes limb weakness and paralysis. While uncommon, AFM affects mostly children, and can have devastating, long-term effects for patients and their families.
There have been three AFM outbreaks in the United States—in 2014, 2016, and 2018. If this biennial pattern continues, another outbreak might occur in 2020.
What AFM Might Look Like
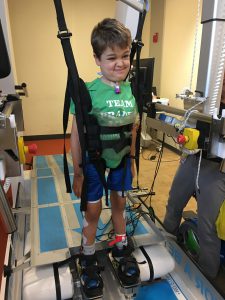
Imagine your 5-year-old son, who is usually very excited to get up and get going in the morning, complains that his neck hurts, and he can’t move his left arm. You think nothing of it. Maybe he just slept wrong and his arm “fell asleep” and it will go away shortly.
You fix his favorite cereal and call him to come eat, but he doesn’t. It’s been almost half an hour since he woke up. Any other morning, he’d be running around, talking about this and that, and demanding his breakfast. You check on him again. He is still lying in bed and still complaining about his neck and arm.
You check his temperature, which seems fine. What could this be? You don’t think he’s making it up, especially since he was excited about an art project happening today.
You call the doctor’s office and get the nurse on the line. She asks you a series of questions, and you remember that his older sister was sick last week with a mild fever, but your son only had some sniffles. Your pediatrician wants to see your son right away, and after examining his reflexes and strength, he tells you to bring your son immediately to the nearest children’s hospital’s emergency department (ED). The pediatrician suspects your son may have a serious neurologic condition. Scared and worried, you rush to the ED.
AFM is a Medical Emergency
AFM can progress quickly to respiratory failure. Patients who develop AFM symptoms need immediate medical care. That’s why it’s very important that parents call their child’s pediatrician right away or go to the ED, and that clinicians recognize the symptoms of AFM early and hospitalize patients for further evaluation and monitoring.
When to Suspect AFM
You should suspect AFM when a person has sudden onset of arm or leg weakness. Also, did the person have a recent respiratory illness or fever? If so, this should heighten your suspicion for AFM.
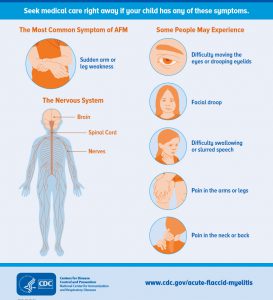
Also, look for other signs and symptoms such as:
- Loss of muscle tone and reflexes in the affected extremities.
- Difficulty moving the eyes or drooping eye lids.
- Facial droop or weakness.
- Difficulty with swallowing or slurred speech.
- Pain in arms or legs.
- Pain in neck or back.
AFM & the COVID-19 Pandemic
COVID-19 is likely on everyone’s minds and causing concern, uncertainty, and challenges for communities across the country.
It is not known how the COVID-19 pandemic and social distancing may affect AFM this year, or the health care system’s ability to promptly recognize and respond to it. However, even in communities with high COVID-19 activity:
- Parents should act and get medical attention immediately if their child develops sudden arm or leg weakness. It may be AFM, which is serious and requires urgent care. It is very likely that the assessment of your child will require hospitalization if clinicians think your child might have AFM.
- Clinicians should not “wait and see.” They should refer patients suspected to have AFM to the ED immediately. They should reference CDC resources on AFM symptoms, provide optimal medical management, collect specimens, and report cases to health departments. Clinicians can also contact an AFM expert for a clinical consult through the AFM Physician Consult and Support Portal.
Clinicians may consider reassuring parents about going to the ED during the COVID-19 pandemic for serious health problems. Clinicians can let parents know that hospitals are taking precautions to prevent exposures to COVID-19, such as providing separate entrances and rooms for those with respiratory symptoms, requiring hospital staff to wear appropriate protective equipment like face coverings and shields for all encounters with patients, and increasing access to hand sanitizer and disinfecting surfaces frequently.
AFM remains a public health priority for CDC. CDC is committed to investigating AFM, working with partners, supporting affected families, and responding to outbreaks. Clinicians are encouraged to review CDC’s AFM website, stay alert for AFM in late summer through fall, and promptly evaluate and hospitalize AFM patients.
Resources for Parents:
- CDC’s webpages for parents of children with AFM
- AFM Fact Sheet
- Diagnosing and Classifying AFM
- Acute Flaccid Myelitis Association
- Seigel Rare Neuroimmune Association
Resources for Health Care Professionals:
- CDC’s AFM webpages for clinicians and health departments
- Watch CDC’s Public Health Grand Rounds about AFM released on July 21, 2020, and earn free continuing education.
If you have questions, you may send them to AFMQuestions@cdc.gov.
Thanks in advance for your questions and comments on this Public Health Matters post. Please note that the CDC does not give personal medical advice. If you are concerned you have a disease or condition, talk to your doctor.
Have a question for CDC? CDC-INFO (http://www.cdc.gov/cdc-info/index.html) offers live agents by phone and email to help you find the latest, reliable, and science-based health information on more than 750 health topics.
3 comments on “AFM is Serious: Know the Symptoms. Act Fast.”
Comments listed below are posted by individuals not associated with CDC, unless otherwise stated. These comments do not represent the official views of CDC, and CDC does not guarantee that any information posted by individuals on this site is correct, and disclaims any liability for any loss or damage resulting from reliance on any such information. Read more about our comment policy ».


Found your post interesting to read. I can’t wait to see your post soon. Good Luck for the upcoming update.This article is really very interesting and effective.
Important to share with caregivers.
Right ! I have 1 child in a chair 24/ 7 born w/ arthogryops
Another son who woke up 1 morning at the age of 2 , he had absolutely no use in right leg until 4 pm or later that the use came back . He was back to amazing 2 year old energetic little boy. Myself im F all the above self meditated for strength .