Reaching Towards a Healthier, Safer Workplace:NIOSH looks at healthcare worker familiarity with recommended respiratory protection practices
Posted on byEvery day healthcare workers (HCWs) make decisions about the best way to protect themselves. What would you do if you entered the room of a new patient and noticed symptoms such as fever and a mucus-producing cough? As a HCW, you must then ask yourself, “What type of disease does the patient have? What sort of precautions should I take to protect myself because the patient may have an infectious disease?” While it is your employer’s responsibility to provide policies, programs, training, and guidance on respirator use, it is the health care workers who implement these procedures. Do you know when to use respiratory protection? If so, do you understand what type of protection to choose and how to use it properly?
NIOSH Research – the REACH II Study
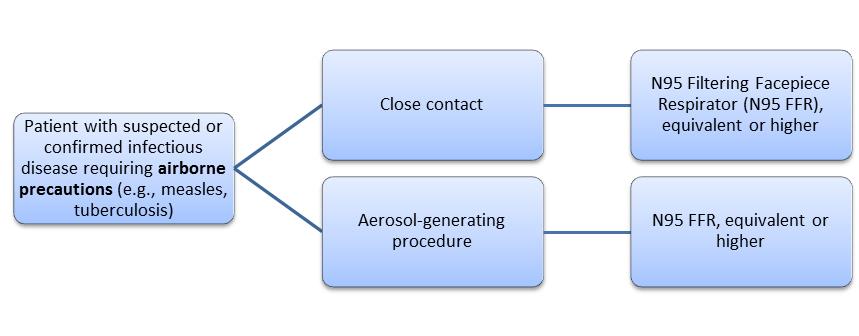
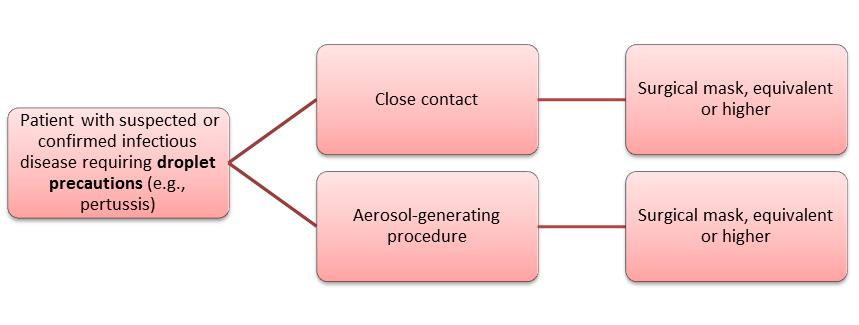
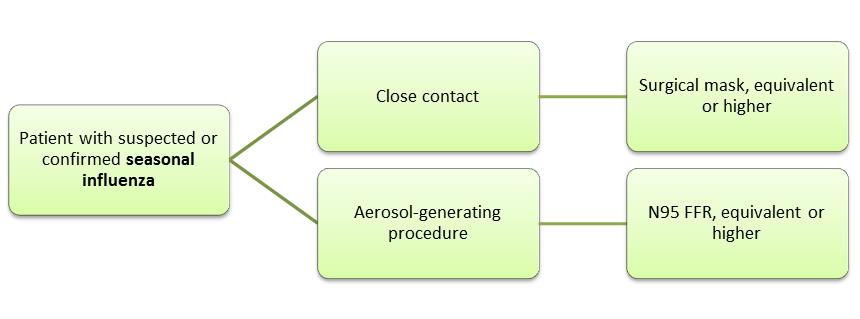
Researchers at NIOSH conducted a study to determine HCW familiarity with recommended respiratory protection practices[i],[ii] including the selection of respiratory protective devices. NIOSH collaborated with several state health departments and universities for the Respirator Use Evaluation in Acute Care Hospitals (REACH II) study. REACH II involved 98 hospitals in six states, and surveyed over 1,500 HCWs, Hospital and Unit Managers. Research staff observed respirator donning (i.e., putting on) and doffing (i.e., taking off) demonstrations by more than 300 HCWs. To determine HCWs’ knowledge about which respiratory protection to use, both HCWs and managers were given six scenarios based on the type of precaution needed (i.e., airborne, droplet or seasonal influenza) and task (i.e., close contact or aerosol-generating procedure). Participants were then asked to choose the minimum type of respiratory protection recommended for each scenario listed below. In most healthcare settings, close contact means that a HCW is within 6 to 10 feet of a potentially infectious patient2. In particular, aerosol-generating procedures2, such as bronchoscopies or endotracheal intubations, can be hazardous for HCWs because they promote the production of sprays or mists that may contain infectious agents.
Results
In the majority of hospitals, NIOSH considered both managers and HCWs knowledgeable about recommended protection for scenarios involving close contact or aerosol-generating procedures on a patient with a suspected or confirmed infectious disease requiring droplet precautions. However, managers and HCWs were least knowledgeable about protection needed for scenarios involving aerosol-generating procedures on patients with suspected or confirmed seasonal influenza. Additionally, HCWs demonstrated a lack of knowledge about scenarios involving close contact or aerosol-generating procedures on patients with a suspected or confirmed infectious disease requiring airborne precautions.
During the donning and doffing observations, many HCWs demonstrated improper techniques:
- 45% used incorrect strap placement
- 85% did not perform a seal check
- 57% did not use straps during doffing
- 45% used incorrect respirator disposal methods
Overall, HCWs were unaware of when to wear respiratory protection, what type is needed in many scenarios, and how to use it properly. Without accurate knowledge, HCWs may choose insufficient protection or use improper methods, which can put their health at risk. To improve HCWs’ knowledge about recommended respiratory protection practices, NIOSH plans to use the REACH II findings to develop useful tools and best practice guidelines. As we develop these tools, we are interested to learn about your experiences with respiratory protection in healthcare settings. Have there been times in which you were unsure about recommended respiratory protection practices? What are your suggestions for improving HCW knowledge on this subject?
To learn more about the REACH II study and respiratory protection in healthcare settings, please visit:
NIOSH Information for Respirator Users
NIOSH Personal Protective Technology Program Healthcare Stakeholder Meeting
Lindsay Stradtman, MPH; Jaclyn Krah, MA; Debra Novak, PhD, RN
Ms. Stradtman is an ASPPH/CDC Public Health Fellow in the NIOSH National Personal Protective Technology Laboratory.
Ms. Krah is a Health Communication Specialist in the NIOSH National Personal Protective Technology Laboratory.
Dr. Novak is a Senior Service Fellow in the NIOSH National Personal Protective Technology Laboratory.
Acknowledgements
NIOSH would like to thank Dr. Lisa Brosseau at the University of Illinois at Chicago School of Public Health and Dr. Kristina Peterson at RTI International for their critical review of this content as well as the REACH II Evaluation Study Group – Lisa M Brosseau, ScD, CIH; Lorraine Conroy, ScD, CIH; Robert Harrison, MD, MPH; Leah Hines, MPH; Elizabeth Rees, MPH; Elizabeth Ritchie, MS; and Bonnie Rogers, DrPH, COHN,-S, LNCC, FAAN .
References
[i] CDC [2013]. Prevention Strategies for Seasonal Influenza in Healthcare Settings. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Immunization and Respiratory Diseases, [http://www.cdc.gov/flu/professionals/infectioncontrol/healthcaresettings.htm].
[ii] Siegel JD, Rhinehart E, Jackson M, Chiarello L, and the Healthcare Infection Control Practices Advisory Committee [2007] Guideline for Isolation Precautions: Preventing Transmission of Infectious Agents in Healthcare Settings [http://www.cdc.gov/hicpac/pdf/isolation/Isolation2007.pdf].
3 comments on “Reaching Towards a Healthier, Safer Workplace:NIOSH looks at healthcare worker familiarity with recommended respiratory protection practices”
Comments listed below are posted by individuals not associated with CDC, unless otherwise stated. These comments do not represent the official views of CDC, and CDC does not guarantee that any information posted by individuals on this site is correct, and disclaims any liability for any loss or damage resulting from reliance on any such information. Read more about our comment policy ».
Nice post. Interesting.
Thanks for sharing.
Very helpful and easy to share with staff.
Fantastic article about the importance of respiratory personal protective equipment. Thank you for sharing this research.